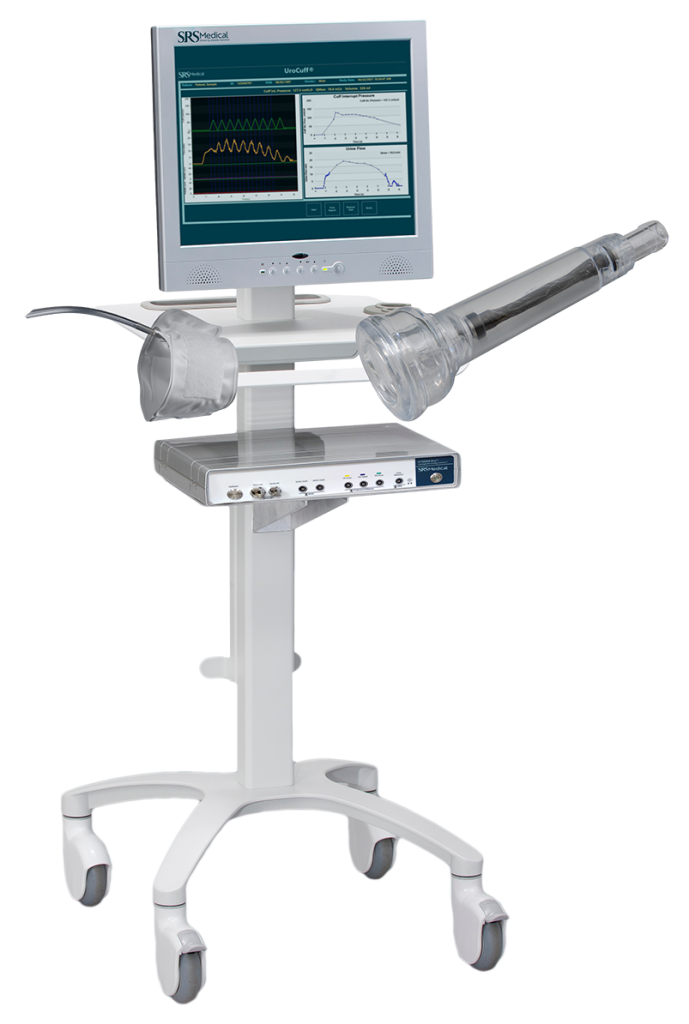
Discover why symptoms like weak stream and straining aren’t enough for accurate BPH diagnosis. Learn how UroCuff® objective testing reduces uncertainty in LUTS management.
The Problem with Symptom-Based BPH Diagnosis
Two patients. Same symptoms. Same IPSS score. Completely different diagnoses.
This is the challenge urologists face when managing lower urinary tract symptoms. Weak stream, straining, or nocturia may point to benign prostatic hyperplasia — but they can also signal neurologic dysfunction, infection, or other causes.
Without objective testing, physicians may treat the wrong condition — and patients may receive unnecessary medication, delayed care, or invasive procedures that won’t help.
Why Symptoms Alone Fall Short in LUTS Diagnosis
Two patients. Same symptoms. Same IPSS score. Completely different diagnoses.
Many practices begin with patient-reported symptom scores like the International Prostate Symptom Score (IPSS). While useful for gauging severity, symptom overlap between conditions makes IPSS an insufficient diagnostic tool.
Common causes of LUTS include:
- Benign prostatic hyperplasia (BPH)
- Neurogenic disorders
- Urethral stricture
- Urinary tract infection
- Pelvic floor dysfunction
- Medication side effects
Key Point: A weak urinary stream does not always equal obstruction.
Treating based on symptoms alone = diagnostic uncertainty.
Case Study: Same Symptoms, Different Diagnoses
Two patients presented with identical symptoms and IPSS scores:
- IPSS: 20
- QOL: 3
Patient A: 79 y/o (download full report)
- Qmax = 9 mL/s
- Max Pressure = 60 cmH₂O
- Vvol: 119mL
- Abdominal Contribution: Significant recruitment throughout void
- Pattern indicates neurogenic component.
Patient B: 59 y/o (download full report)
- Qmax = 12 mL/s
- Max Pressure = 200 cmH₂O
- Vvol: 244mL
- Abdominal Contribution: Minimal recruitment to initiate void, none throughout
- Pattern indicates clear obstruction.
Without UroCuff, both may have received the same therapy. With UroCuff, each patient received tailored care — one directed toward neurologic protocol, the other toward surgical protocol.
Benefits of UroCuff in Clinical Decision-Making
Implementing objective diagnostics like UroCuff transforms practice in several ways:
- Reduces diagnostic uncertainty.
- Improves patient trust with visual, data-driven results.
- Guides therapy (α-blockers, MIST, HoLEP, CIC, or advanced diagnostics).
- Optimizes outcomes by matching the right treatment to the right patient.
Conclusion: Stop Assuming, Start Measuring
In BPH and LUTS management, symptoms alone can mislead. The UroCuff® Test with PVR provides clear, objective data that supports more confident decisions, better outcomes, and stronger patient relationships.
Learn more about how UroCuff can enhance your practice at urocuff.com.
The Role of Initial Diagnostics in Evaluating Patients with Lower Urinary Tract Symptoms
Justin Cohen, MD
UroPartners, Chicago, IL
“When a patient presents with complaints such as weak urinary stream and straining, it is essential to determine the underlying etiology before initiating treatment. These symptoms can arise from multiple causes, and initial therapies will vary depending on the precise diagnosis. The quality of the first evaluation not only directs appropriate treatment but also influences whether the patient remains engaged in their care or is lost to follow-up.
Patients who seek help for urinary symptoms come with clear expectations that their concerns will be understood and addressed in a timely and effective manner. Without appropriate initial diagnostics, there is a risk of wasted time, patient frustration, and potential digression into ineffective or unnecessary treatments. Objective evaluation at the outset is therefore critical to guiding management and ensuring patient confidence in the care process.
For a true differential diagnosis of lower urinary tract symptoms, both pressure and flow measurements are required to clarify the etiology. The UroCuff Test provides this essential information in a non-invasive manner, without the pain, discomfort, or procedural impact associated with more invasive urodynamic studies.
The UroCuff delivers two complementary sets of information:
- Bladder Pressure Profile: Evaluates bladder contractility, bladder capacity, efficiency of micturition, while identifying abdominal recruitment.
- Flow Parameters: Defines maximum and average urinary flow rates, flow time, and flow pattern.
By analyzing the relationship between pressure and flow, the UroCuff Test helps clarify the etiology of the patient’s symptoms and provides a reliable foundation for clinical decision-making.
With objective UroCuff data, an effective and individualized treatment pathway can be established. For example:
- If the UroCuff demonstrates elevated pressure with restricted flow, the next step would involve advanced diagnostics to identify the appropriate minimally invasive de-obstructive procedure.
- Conversely, if the UroCuff indicates compromised bladder function with poor flow parameters, the patient may be referred for pelvic floor therapy and managed within a neurogenic bladder protocol.
Objective diagnostics in LUTS assessment ensures that therapy is evidence-based, patient-centered, and directed toward the most effective outcome.“
Justin Cohen, MD
UroPartners, Chicago, IL
Your Bladder Matters
Ask your urologist about your bladder function test results.
Better Answers
The UroCuff Test measures bladder function during voiding and provides important insights to optimize BPH care.
It offers your practice a LUTS patient management platform providing better clinical outcomes and greater efficiency.